Ultrasound & Transvaginal Sonography
Uvaginal ltrasound & TransSonography
Ultrasound Sonography
Sonography is a noninvasive, painless procedure. It uses high-frequency sound waves — called ultrasound waves —to produce images of organs, soft tissues, blood vessels, and blood flow, from inside the body. These images are used for medical analysis.
fter x-ray exams, ultrasound is the most commonly used form of diagnostic imaging. It helps doctors gain insights into the inner workings of the body, and is known for being:
- Safe
- Radiation free
- Noninvasive
- Portable
- Widely accessible
- Affordable
Sonogram
A sonogram (also called an ultrasonogram) is the visual image produced during an ultrasound examination.
Transvaginal sonography What is a transvaginal ultrasound?
An ultrasound test uses high-frequency sound waves to create images of your internal organs. Imaging tests can identify abnormalities and help doctors diagnose conditions.
A transvaginal ultrasound, also called an endovaginal ultrasound, is a type of pelvic ultrasound used by doctors to examine female reproductive organs. This includes the uterus, fallopian tubes, ovaries, cervix, and vagina.
“Transvaginal” means “through the vagina.” This is an internal examination.
Unlike a regular abdominal or pelvic ultrasound, where the ultrasound wand (transducer) rests on the outside of the pelvis, this procedure involves your doctor or a technician inserting an ultrasound probe about 2 or 3 inches into your vaginal canal.
When is a transvaginal ultrasound performed?
There are many reasons why a transvaginal ultrasound might be necessary, including:
- an abnormal pelvic or abdominal exam
- unexplained vaginal bleeding
- pelvic pain
- an ectopic pregnancy (which occurs when the fetus implants outside of the uterus, usually in the fallopian tubes)
- infertility
- a check for cysts or uterine fibroids
- verification that an IUD is placed properly
- monitor the heartbeat of the fetus
- look at the cervix for any changes that could lead to complications such as miscarriage or premature delivery
- examine the placenta for abnormalities
- identify the source of any abnormal bleeding
- diagnose a possible miscarriage
- confirm an early pregnancy
How should I prepare for a transvaginal ultrasound?
In most cases, a transvaginal ultrasound requires little preparation on your part.
Once you’ve arrived at your doctor’s office or the hospital and you’re in the examination room, you have to remove your clothes from the waist down and put on a gown.
Depending on your doctor’s instructions and the reasons for the ultrasound, your bladder might need to be empty or partially full. A full bladder helps lift the intestines and allows for a clearer picture of your pelvic organs.
Ovulation Induction & IUI
Ovulation induction is a straightforward fertility treatment that involves taking oral or injectable medication to stimulate regular ovulation. The medication is usually taken at the beginning of the menstrual cycle and the body’s response is monitored through the cycle using ultrasound.
Ovulation induction uses fertility medications to stimulate the release of one or more eggs from the ovary. Sometimes, a procedure called intrauterine insemination (IUI) is used in conjunction with ovulation induction to achieve pregnancy.
Intrauterine insemination (IUI) — a type of artificial insemination — is a procedure for treating infertility.
Sperm that have been washed and concentrated are placed directly in your uterus around the time your ovary releases one or more eggs to be fertilized.
The hoped-for outcome of intrauterine insemination is for the sperm to swim into the fallopian tube and fertilize a waiting egg, resulting in a normal pregnancy. Depending on the reasons for infertility, IUI can be coordinated with your normal cycle or with fertility medications.
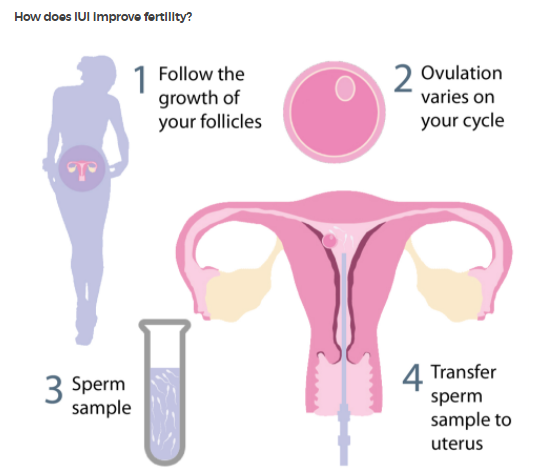
Why it's done
A couple’s ability to become pregnant depends on many different factors. Intrauterine insemination is used most often in couples who have:
- Donor sperm. For women who need to use donor sperm to get pregnant, IUI is most commonly used to achieve pregnancy. Frozen donor sperm specimens are obtained from certified labs and thawed before the IUI procedure.
- Unexplained infertility. IUI is often performed as a first treatment for unexplained infertility along with ovulation-inducing medications.
- Endometriosis-related infertility. For infertility related to endometriosis, using medications to obtain a good-quality egg along with performing IUI is often the first treatment approach.
- Mild male factor infertility (subfertility). Your partner’s semen analysis, one of the first steps in the medical assessment of infertility, may show below-average sperm concentration, weak movement (motility) of sperm, or abnormalities in sperm size and shape (morphology). IUI can overcome some of these problems because preparing sperm for the procedure helps separate highly motile, normal sperm from those of lower quality.
- Cervical factor infertility. Your cervix, at the lower end of the uterus, provides the opening between your vagina and uterus. Mucus produced by the cervix around the time of ovulation provides an ideal environment for sperm to travel from your vagina to the fallopian tubes. But, if your cervical mucus is too thick, it may impede the sperm’s journey. The cervix itself may also prevent sperm from reaching the egg. Scarring, such as that caused by a biopsy or other procedures, can cause the cervix to thicken. IUI bypasses your cervix, depositing sperm directly into your uterus and increasing the number of sperm available to meet the awaiting egg.
- Ovulatory factor infertility. IUI may also be performed for women who have infertility caused by problems with ovulation, including an absence of ovulation or a reduced number of eggs.
- Semen allergy. Rarely, a woman could have an allergy to proteins in her partner’s semen. Ejaculation into the vagina causes redness, burning and swelling where the semen contacts the skin. A condom can protect you from the symptoms, but it also prevents pregnancy. If your sensitivity is severe, IUI can be effective, since many of the proteins in semen are removed before the sperm is inserted.

